This article was co-authored by Joel Giffin, PT, DPT, CHT. Dr. Joel Giffin is a Doctor of Physical Therapy and the Founder of Flex Physical Therapy in New York, New York. With over 15 years of experience as a Certified Hand Therapist (CHT), Dr. Giffin treats the whole body and specializes in rehabilitation of the hand and upper extremities. He has treated Broadway theater performers backstage at shows such as The Lion King, Sleep No More, Tarzan, and Sister Act. Flex Physical Therapy also specializes in occupational and pelvic floor therapy. Dr. Giffin earned his Master’s degree in Physical Therapy with honors from Quinnipiac University and received his Doctor of Physical Therapy (DPT) degree with distinction from Simmons College. He is a member of the American Physical Therapy Association and the American Society of Hand Therapists.
There are 8 references cited in this article, which can be found at the bottom of the page.
This article has been viewed 6,413 times.
Degenerative joint disease, also known as osteoarthritis, is a medical condition that can affect many different joints, including those in the lower back. This condition causes the cartilage that protects the joints to break down, which can cause pain and swelling.[1] You may be able to recognize many of the symptoms of degenerative joint disease on your own, but if you suspect that you have it, it's important to see a doctor for a formal diagnosis. Once you have been diagnosed, your doctor can help you decide what kind of treatment would be best for you.
Steps
Part 1
Part 1 of 2:Recognizing Symptoms
-
1Note the location of pain. Pain is often the most noticeable symptom of joint disease. If you suffer from degenerative joint disease in your lower back, you may notice pain in any of the following areas:[2]
- In the back
- In the buttock
- Radiating down the back, sides, or front of your legs
-
2Pay attention to your mobility. Degenerative joint disease can affect the function of the joint, in addition to causing pain. If you have this condition, you may notice a number of changes in the way you are able to move your body.[3]
- You may experience pain when moving, so sitting may be more comfortable than standing.
- You may not be able to bend, twist, squat, or lift things the same way you used to.[4]
- You may find that your body is very stiff and rigid, especially after you have rested. This may be one of the earliest signs you notice.[5]
- Your legs may feel weak, which can make moving more difficult.[6]
-
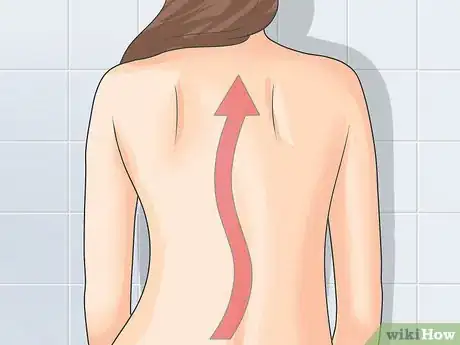
3Look for changes in appearance. Degenerative joint disease sometimes causes noticeable changes in the appearance of the body, although the changes may be subtle. Pay close attention to your body and make note of any changes you observe.[7]
- You may have visible swelling in the affected area.
- The normal curve of your spine may change or even disappear.
-
4Listen for new sounds. Some people who have degenerative joint disease of the spine experience an audible cracking or crunching of the joints. If you hear these kinds of sounds, it may be caused by your bones rubbing against each other due to a lack of cartilage.
-
5Be aware of spasms. Some people who suffer from degenerative joint disease experience muscle spasms. These may be uncomfortable and may force you to change your sitting position.[8]
-
6Know what symptoms may indicate a different condition. There are a variety of different conditions that can cause symptoms like back pain, numbness and weakness. You may be able to rule out degenerative joint disease if you experience certain symptoms that are indicative of other conditions.
- If the skin around the affected area is red or feels hot, you are more likely suffering from rheumatoid arthritis.
- If you felt a popping sensation before you began experiencing pain, you are more likely suffering from sciatica.[9]
- If you experienced trauma of any kind, you may have an acute injury to your spine, such as a fracture.
-
7Understand the risk factors. While degenerative joint disease can happen to anyone, it is much more common in older individuals, as the body's cartilage tends to degrade over a long period of time. Joint degeneration is also much more common in individuals with a history of the following:
- Obesity
- Compromised immune system
- Malnutrition
- Congenital joint disorders
- Prolonged abuse of joints (from poor posture, sports, or work-related activities)
Part 2
Part 2 of 2:Getting a Medical Diagnosis
-
1See your doctor. If you are experiencing any of the above symptoms, you should schedule an appointment with a doctor as soon as possible. Only a doctor can determine if your symptoms are indeed being caused by degenerative joint disease of the lower back.[10]
- Your visit will likely include a physical examination and a review or your medical history.
- Your doctor may want to do blood tests to rule out other possible causes of your symptoms, such as infection.
-
2Undergo manipulation tests. Sometimes, doctors must manipulate the body in order to diagnose a problem. Doctors use specific tests that have been designed to isolate certain joints. While these tests may be a bit uncomfortable, they should not cause any further damage to your joints.[11]
- For example, the FABER test, which doctors perform by rotating the hip externally while the patient is lying supine, is excellent for identifying joint disease in the sacroiliac joint, which is located between the spine and the pelvis.
-
3Get an x-ray. One of the first tests your doctor will likely order is an x-ray. This can help reveal any abnormalities that involve the bone, including fractures or growths.[12]
- Bone spurs are a common complication of degenerative joint disease, and these will be visible on an x-ray. However, keep in mind that degenerative changes on an x-ray do not automatically mean that your pain is because of these degenerative changes. Approximately 90 percent of people over the age of 64 have degenerative changes, which indicates that degenerative changes are a part of ageing.[13]
-
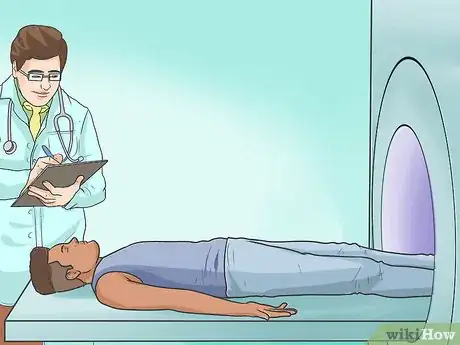
4Get an MRI. While x-rays are helpful for seeing what is happening with the bone, they do not show soft tissue. Your doctor may order an MRI in addition to or instead of an x-ray. This test will help reveal abnormalities in the discs and nerve roots. [14]
- While x-rays use radiation to produce images, MRIs use magnetic force.
-
5Be prepared for other imaging tests. While x-rays and MRIs are the most common imaging tests used to diagnose lower back pain, there are a variety of other tests that your doctor may want to perform. Additional tests are particularly likely if your x-ray and/or MRI fail to reveal the source of your symptoms.[15]
- CT scans are used to create three-dimensional images of your spine, including soft tissue.
- Myelograms enhance traditional x-rays or CT scans by using an injectable dye to increase contrast.
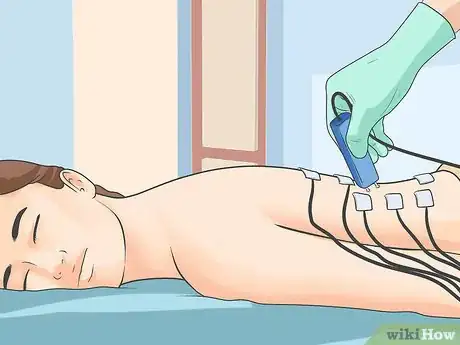
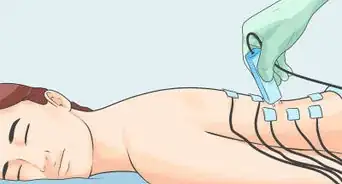
- EMGs use small needles to measure electrical activity in the muscles, which helps doctors diagnose nerve damage.
- Bone scans use a small amount of injectable radioactive material and a scanner to take images of the bones, which helps doctors assess the extent of a patient's joint disease.
-
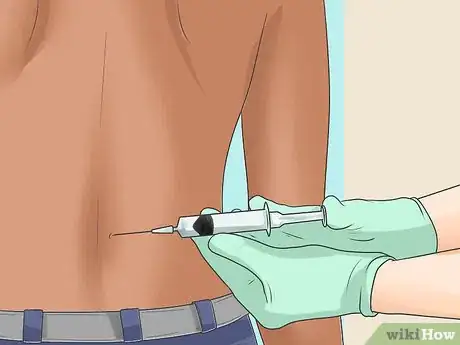
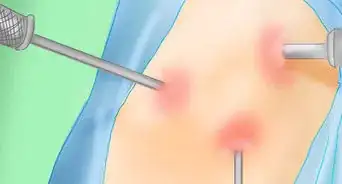
6Have an injection test. Your doctor may inject a numbing medication into one of your joints in order to determine definitively which joint is causing your symptoms. This is especially helpful if other tests have been inconclusive or if there are multiple possible causes of your pain.[16]
- This test works by temporarily relieving your pain. If you get effective pain relief, the offending joint has been identified. If you do not get pain relief, your problem is being caused by a different joint.
-
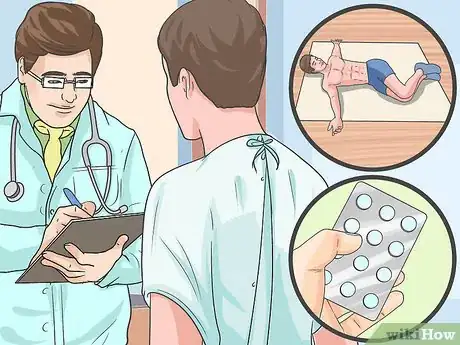
7Get treated. Once your condition has been diagnosed, you can work with your doctor to determine the best course of treatment. There are a variety of treatments available to help patients with degenerative joint disease, and the right one for you will depend on the severity of your condition, your medical history, and many other factors.[17]
- Your doctor may prescribe medication to reduce pain, swelling, and muscle spasms.
- Your doctor may recommend that you receive treatment from a chiropractor or physical therapist.
- You may be given a TENS device, which attaches to the skin and provides electrical stimulation that can block pain.
- Alternative pain management options, such as acupuncture and biofeedback, may also be available.
- Your doctor may recommend that you have injections to reduce your pain. Epidural steroid injections are commonly used for temporary relief, and nerve block therapies may provide more permanent relief.
- Your doctor may also recommend an exercise program, most likely through a physical therapist. An exercise program can help to strengthen and increase the flexibility of the muscles around your back joints, which may help to reduce pain and discomfort. It may take several weeks for you to see any effect from these exercises, so try to be patient.
- If no other treatment methods are successful, your doctor may recommend that you have back surgery. There are a variety of different procedures that can be performed, depending on the exact source of your pain.
Expert Q&A
Did you know you can get expert answers for this article?
Unlock expert answers by supporting wikiHow
-
QuestionWhat are some symptoms of osteoarthritis in the lower back?
 Joel Giffin, PT, DPT, CHTDr. Joel Giffin is a Doctor of Physical Therapy and the Founder of Flex Physical Therapy in New York, New York. With over 15 years of experience as a Certified Hand Therapist (CHT), Dr. Giffin treats the whole body and specializes in rehabilitation of the hand and upper extremities. He has treated Broadway theater performers backstage at shows such as The Lion King, Sleep No More, Tarzan, and Sister Act. Flex Physical Therapy also specializes in occupational and pelvic floor therapy. Dr. Giffin earned his Master’s degree in Physical Therapy with honors from Quinnipiac University and received his Doctor of Physical Therapy (DPT) degree with distinction from Simmons College. He is a member of the American Physical Therapy Association and the American Society of Hand Therapists.
Joel Giffin, PT, DPT, CHTDr. Joel Giffin is a Doctor of Physical Therapy and the Founder of Flex Physical Therapy in New York, New York. With over 15 years of experience as a Certified Hand Therapist (CHT), Dr. Giffin treats the whole body and specializes in rehabilitation of the hand and upper extremities. He has treated Broadway theater performers backstage at shows such as The Lion King, Sleep No More, Tarzan, and Sister Act. Flex Physical Therapy also specializes in occupational and pelvic floor therapy. Dr. Giffin earned his Master’s degree in Physical Therapy with honors from Quinnipiac University and received his Doctor of Physical Therapy (DPT) degree with distinction from Simmons College. He is a member of the American Physical Therapy Association and the American Society of Hand Therapists.
Physical Therapist In the beginning, it sometimes starts off as stiffness, even more so than any pain. As things develop, it tends to turn into pain in the lower back, glute muscles, butt muscles, and even in the side or front of the legs. You might also notice a limited ability to bend, squat, lift, or stand up from the floor.
In the beginning, it sometimes starts off as stiffness, even more so than any pain. As things develop, it tends to turn into pain in the lower back, glute muscles, butt muscles, and even in the side or front of the legs. You might also notice a limited ability to bend, squat, lift, or stand up from the floor.
References
- ↑ http://www.webmd.com/osteoarthritis/guide/spinal-osteoarthritis-degenerative-arthritis-of-the-spine
- ↑ Joel Giffin, PT, DPT, CHT. Physical Therapist. Expert Interview. 22 October 2020.
- ↑ http://twinboro.com/body/spine/lumbar/joint/conditions/lumbar-spine-degenerative-joint-disease-nj.html
- ↑ Joel Giffin, PT, DPT, CHT. Physical Therapist. Expert Interview. 22 October 2020.
- ↑ Joel Giffin, PT, DPT, CHT. Physical Therapist. Expert Interview. 22 October 2020.
- ↑ http://www.webmd.com/osteoarthritis/guide/spinal-osteoarthritis-degenerative-arthritis-of-the-spine
- ↑ http://twinboro.com/body/spine/lumbar/joint/conditions/lumbar-spine-degenerative-joint-disease-nj.html
- ↑ http://twinboro.com/body/spine/lumbar/joint/conditions/lumbar-spine-degenerative-joint-disease-nj.html
- ↑ http://www.medicinenet.com/degenerative_disc/page3.htm
- ↑ http://www.webmd.com/osteoarthritis/guide/spinal-osteoarthritis-degenerative-arthritis-of-the-spine?page=2
- ↑ http://spinecenter.ucla.edu/sacroiliac-joint-disease
- ↑ http://www.webmd.com/osteoarthritis/guide/spinal-osteoarthritis-degenerative-arthritis-of-the-spine
- ↑ http://www.ncbi.nlm.nih.gov/pubmed/2146754
- ↑ http://twinboro.com/body/spine/lumbar/joint/conditions/lumbar-spine-degenerative-joint-disease-nj.html
- ↑ http://www.ninds.nih.gov/disorders/backpain/detail_backpain.htm#3102_6
- ↑ http://spinecenter.ucla.edu/sacroiliac-joint-disease
- ↑ http://www.ninds.nih.gov/disorders/backpain/detail_backpain.htm#3102_6






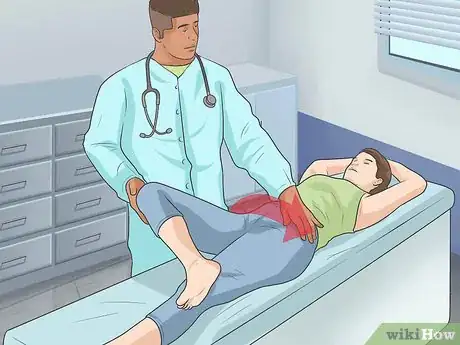












































Medical Disclaimer
The content of this article is not intended to be a substitute for professional medical advice, examination, diagnosis, or treatment. You should always contact your doctor or other qualified healthcare professional before starting, changing, or stopping any kind of health treatment.
Read More...