This article was co-authored by Lydia Shedlofsky, DO. Dr. Lydia Shedlofsky is a Resident Dermatologist who joined Affiliated Dermatology in July of 2019 after completing a traditional rotating internship at Larkin Community Hospital in Miami, Florida. She earned a Bachelor of Science in Biology at Guilford College in Greensboro, North Carolina. After graduation, she moved to Beira, Mozambique, and worked as a research assistant and intern at a free clinic. She completed a Post-Baccalaureate program and subsequently earned a Master's Degree in Medical Education and a Doctorate of Osteopathic Medicine (DO) from the Lake Erie College of Osteopathic Medicine.
There are 12 references cited in this article, which can be found at the bottom of the page.
Scleroderma is a relatively rare disease that causes skin and other body tissue to thicken. While there is no cure for scleroderma, there are many treatments that can ease your symptoms and greatly improve your quality of life. If you're concerned that you might have scleroderma, we've got you covered with all the information you need about how the disease is diagnosed and treated.[1]
Steps
Question 1
Question 1 of 6:Background and Cause
-
1Scleroderma is a type of chronic autoimmune disorder. When you have scleroderma, your immune system mistakenly attacks and damages healthy tissues. This leads to the buildup of hardened, scar-like tissue in your skin and other parts of your body.[2]
- Scleroderma is also a rheumatic disease that can cause inflammation, pain, swelling, and stiffness in joints and tendons.
- Scleroderma isn't an infection or type of cancer, and it isn't contagious.[3]
-
2The condition can be either localized or systemic. Localized scleroderma, also called "morphea," only affects the skin. Systemic scleroderma, or "sclerosis," affects large areas of the skin as well as your internal organs.[4]
- Localized scleroderma typically affects the skin on the chest or abdomen and sometimes on your arms, legs, hands, or feet. It rarely spreads to other parts of the body, meaning it's unlikely that localized scleroderma will turn into systemic scleroderma over time.
-
3Scleroderma is relatively rare. Only about 300,000 people in the US have scleroderma—most of them women between the ages of 30 and 50. While men can also contract the disease, they're much less likely to get it than women.[5]
-
4The exact cause of scleroderma is unknown. A buildup of collagen in the skin and other organs leads to scleroderma, but doctors aren't sure why this happens. Scleroderma sometimes occurs in conjunction with other autoimmune disorders.[6]
Question 2
Question 2 of 6:Symptoms
-
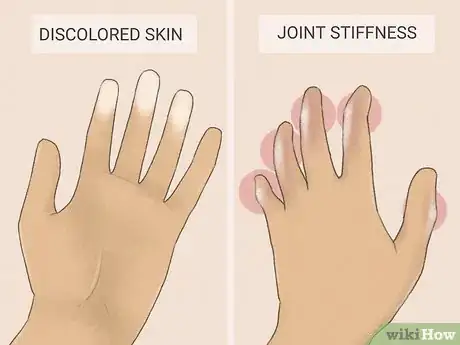
1Symptoms vary depending on which part of the body is affected. Hard, thick, tight skin is the hallmark of scleroderma. Other symptoms may develop depending on where that skin is located. These symptoms include:[9]
- Hair loss
- Dry, itchy skin
- Discolored skin (occasionally a salt-and-pepper look, which might be a sign of systemic scleroderma)
- Joint stiffness and inflammation
- Muscle shortening and weakness
-
2Your fingers and toes may turn blue or go numb. This condition is called Raynaud's disease, in which the small blood vessels in your fingers and toes contract. This happens in response to cold temperatures or emotional distress.[10]
- Raynaud's disease also occurs in people who don't have scleroderma. However, it's one of the first signs that you might have systemic scleroderma.
-
3Some symptoms indicate your internal organs are affected. If you have systemic scleroderma, it can affect your internal organs. Without treatment, some of these symptoms may be life-threatening. Signs that scleroderma is affecting an internal organ include:[11]
- Heartburn
- Diarrhea
- Constipation
- High blood pressure
- Abnormal heartbeat
- Shortness of breath
- Lack of sex drive
Question 3
Question 3 of 6:Diagnosis
-
1See a dermatologist or rheumatologist for diagnosis. Dermatologists diagnose diseases that affect the skin, while rheumatologists diagnose diseases that affect the joints, muscles, and bones.[12] Both have experience with scleroderma.[13]
- It can take time to get a diagnosis, so be patient. Online support groups might be able to recommend a doctor who has experience with the disease.
-
2Dermatologists usually diagnose scleroderma through a skin biopsy. The dermatologist removes a small piece of your skin that has hardened or thickened and looks at it under a microscope. While the biopsy can't tell the dermatologist if you have scleroderma, it can help them rule out other possibilities.[14]
- Based on the results of the biopsy, the dermatologist might order additional tests or refer you to another specialist for examination.
-
3Blood tests, X-rays, and other tests also help diagnose scleroderma. Unfortunately, there's no single medical test that can tell a doctor definitively if you have scleroderma. All of these tests help your doctor eliminate other possibilities.[15]
- With a blood test, your doctor will look for elevated antinuclear antibodies. Although people with other diseases also have this, it occurs in 95% of scleroderma patients.
Question 4
Question 4 of 6:Treatment
-
1Physical and occupational therapy work best if started early. Physical and occupational therapy help you keep your range of motion in your joints and reduce stiffness. They can also reduce the tightness of your skin over your joints. However, if you've already lost a good bit of your range of motion when you start therapy, you'll be less likely to get it back.[16]
-
2A dermatologist can treat skin problems. If your scleroderma primarily affects your skin, go to a dermatologist for treatment. They'll determine how deeply your skin is hardened and recommend treatment options based on that. They might try:[17]
- Lotions or moisturizers
- Corticosteroids
- Camphor or menthol (for itchiness)
- Intense pulsed light (IPL) treatments (for discolored skin)
- UVA treatment
- Laser therapy (for visible blood vessels)
-
3Medication might be prescribed to manage symptoms. Depending on how scleroderma affects you, your doctor might prescribe medications to provide some relief. Drugs that benefit scleroderma patients are designed to:[18]
- Suppress the immune system
- Control blood pressure
- Decrease inflammation
- Manage digestive tract function
- Relieve heartburn
-
4Surgery can be used as a last resort. If you have systemic scleroderma, it usually gets worse over time and can cause other complications. If your symptoms aren't well-managed with medication, your doctor might recommend surgery. This is very rare.[19]
- Some scleroderma patients have fingers amputated if the fingertip tissue begins to die due to advanced Raynaud's disease.
- If you develop severe lung problems, a lung transplant might be necessary.
Question 5
Question 5 of 6:Prognosis
-
1There is no known cure for scleroderma. The US Food and Drug Administration (FDA) hasn't approved any drugs specifically to treat scleroderma. All treatments revolve around easing symptoms, but they don't make the disease itself go away.[20]
- Some immune suppression medications can slow the progression of scleroderma, but they don't stop it completely and the condition will return if you stop taking the medication.
-
2Most scleroderma patients have a normal life expectancy. Despite being a chronic condition, scleroderma doesn't typically cause you to die any earlier than you would if you didn't have it. However, it can cause more stress than usual.[21]
-
3Scleroderma requires continual medical care to manage symptoms. If you've been diagnosed with scleroderma, always be open with your doctor about your symptoms and how you're feeling. Even something minor can develop into something more serious if it isn't addressed promptly.[22]
- Your condition may stabilize and the disease might go into short- or even long-term remission. However, you should still see your doctor on a regular basis and monitor your symptoms closely.
- Skin problems may fade on their own in 2-5 years.[23]
Question 6
Question 6 of 6:Additional Info
-
1Join a support group to help cope. Online and local support groups give you the opportunity to commiserate with others who have scleroderma. This is a place to share jokes, stories, and news about promising treatments.[24]
- Because stress can impact scleroderma's severity, stress-management techniques are extremely important. Other patients can share methods that have worked for them.[25]
-
2Take an active part in maintaining your own health. While your doctors can prescribe medications and offer other treatments that help you manage your symptoms, you have a role to play as well. Self-help strategies for scleroderma patients include:[26]
- Dress in layers to keep warm
- Avoid cold and wet environments
- Quit smoking
- Wear rubber gloves when using household cleaners
- Get regular exercise
-
3Keep your skin clean and protected. If you have scleroderma, your skin is dry and fragile—especially the hardened, thick skin in affected areas. Wash your skin gently and apply moisturizer immediately, then cover it with clothing to keep it warm.[27]
- Because tattoos injure the skin, dermatologists advise against getting a tattoo if you have scleroderma.
-
4Talk to your doctor if you want to try to become pregnant. While you can become pregnant if you have scleroderma, there is a slightly heightened risk of miscarriage. Your doctor can evaluate your current symptoms and advise if getting pregnant is a good idea for you.[28]
- Younger women with scleroderma are at greater risk of infertility compared to older women who've already had children.
- Pregnancy poses greater risks if you have systemic scleroderma than if you have localized scleroderma.
References
- ↑ https://www.mayoclinic.org/diseases-conditions/scleroderma/symptoms-causes/syc-20351952
- ↑ https://medlineplus.gov/ency/article/000429.htm
- ↑ https://www.aad.org/public/diseases/a-z/scleroderma-causes
- ↑ https://medlineplus.gov/ency/article/000429.htm
- ↑ https://www.hopkinsmedicine.org/health/conditions-and-diseases/scleroderma
- ↑ https://medlineplus.gov/ency/article/000429.htm
- ↑ https://www.aad.org/public/diseases/a-z/scleroderma-causes
- ↑ https://www.aad.org/public/diseases/a-z/scleroderma-causes
- ↑ https://www.aad.org/public/diseases/a-z/scleroderma-symptoms
- ↑ https://www.mayoclinic.org/diseases-conditions/scleroderma/symptoms-causes/syc-20351952
- ↑ https://www.aad.org/public/diseases/a-z/scleroderma-symptoms
- ↑ Lydia Shedlofsky, DO. Dermatologist. Expert Interview. 14 May 2021.
- ↑ https://www.aad.org/public/diseases/a-z/scleroderma-treatment
- ↑ https://www.aad.org/public/diseases/a-z/scleroderma-treatment
- ↑ https://www.aad.org/public/diseases/a-z/scleroderma-treatment
- ↑ https://www.aad.org/public/diseases/a-z/scleroderma-treatment
- ↑ https://www.aad.org/public/diseases/a-z/scleroderma-treatment
- ↑ https://www.hopkinsmedicine.org/health/conditions-and-diseases/scleroderma/scleroderma-treatment
- ↑ https://www.mayoclinic.org/diseases-conditions/scleroderma/diagnosis-treatment/drc-20351957
- ↑ https://www.aad.org/public/diseases/a-z/scleroderma-treatment
- ↑ https://www.hopkinsmedicine.org/health/conditions-and-diseases/scleroderma/scleroderma-treatment
- ↑ https://www.hopkinsmedicine.org/health/conditions-and-diseases/scleroderma/scleroderma-treatment
- ↑ https://www.mayoclinic.org/diseases-conditions/scleroderma/diagnosis-treatment/drc-20351957
- ↑ https://www.niams.nih.gov/health-topics/scleroderma#tab-living-with
- ↑ https://www.hopkinsmedicine.org/health/conditions-and-diseases/scleroderma/scleroderma-treatment
- ↑ https://www.niams.nih.gov/health-topics/scleroderma#tab-living-with
- ↑ https://www.aad.org/public/diseases/a-z/scleroderma-self-care
- ↑ https://www.sruk.co.uk/scleroderma/managing-scleroderma/pregnancy/#pregnancy1/page1























































Medical Disclaimer
The content of this article is not intended to be a substitute for professional medical advice, examination, diagnosis, or treatment. You should always contact your doctor or other qualified healthcare professional before starting, changing, or stopping any kind of health treatment.
Read More...