This article was co-authored by Muhammad Khan, MD, MPH and by wikiHow staff writer, Janice Tieperman. Dr. Muhammad Khan is a Gastroenterologist, with over 10 years of experience. Dr. Khan specializes in Pediatric Gastroenterology, Hepatology, and Nutrition, and has a special focus in Therapeutic Endoscopy. He received his Bachelor’s, Master’s, and Doctorate of Medicine degrees from The University of Utah. Dr. Khan completed his residency training at Eastern Virginia Medical School, where he was inducted into the prestigious Alpha Omega Alpha honor society. He then completed his fellowship training at Lucile Packard Children’s Hospital at Stanford University. He is a Fellow of both the American Society of Gastrointestinal Endoscopy (ASGE) and the North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition (NASPGHAN).
There are 16 references cited in this article, which can be found at the bottom of the page.
This article has been viewed 1,371 times.
Depending on your lifestyle or family history, liver fibrosis, or scarring, may be a very real and valid concern for you. Try not to worry—although it’s a serious condition, liver fibrosis on its own is not life-threatening.[1] With the proper precautions and medical advice, liver fibrosis is really easy to understand and identify. To help you get started, here are a few answers to some of your frequently-asked questions.
Steps
Question 1
Question 1 of 8:What is liver fibrosis?
-
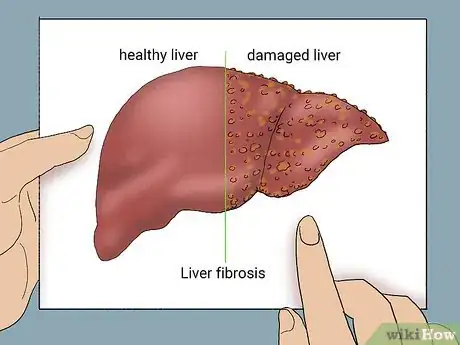
1Liver fibrosis happens when a lot of scar tissue grows on your liver. The liver repairs itself whenever it gets damaged. When the liver gets damaged over and over again, scar tissue grows instead of regular, healthy tissue—this is known as fibrosis.[2] [3]
- Unfortunately, scarred liver tissue doesn’t work as well as healthy tissue.[4]
Advertisement
Question 2
Question 2 of 8:What causes liver fibrosis?
-
1Alcohol abuse can cause liver fibrosis. One of the liver’s main jobs is breaking down and clearing out any toxins in your blood. Whenever you enjoy an alcoholic drink, your liver filters out the alcohol from your bloodstream. If a person drinks too much, liver cells can get destroyed, which leads to scarring.[5] [6] Because of this, alcohol abuse is closely associated with liver fibrosis.[7]
-
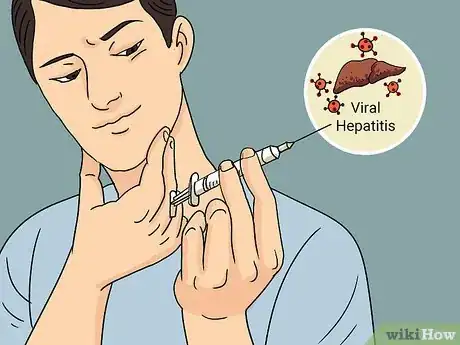
2Viral hepatitis C can lead to liver fibrosis.[8] Hepatitis C spreads through infected blood and causes a liver infection, which can lead to scarring. Don’t worry—while there isn’t a vaccine for this virus, you’re much less likely to catch it as long as you don’t share needles and other personal items with people.[9]
-
3Nonalcoholic fatty liver may cause liver fibrosis. This condition is more common with people who are overweight, diabetic, or prediabetic, as well as people with high cholesterol.[12] Sometimes, people with nonalcoholic fatty liver develop liver inflammation, which can turn into scarring.[13] It’s okay—with a doctor’s guidance, this condition is very manageable and treatable.[14]Advertisement
Question 3
Question 3 of 8:What are the symptoms of liver fibrosis?
Question 4
Question 4 of 8:Who is most at risk for liver fibrosis?
-
1People who take certain supplements and medications might be at risk.[17] Pills like acetaminophen (Tylenol), aloe vera, antidepressants, anticonvulsants, and many more can lead to liver damage. To be safe, always check with a doctor before taking any new medications or supplements.[18]
- For a full list of supplements and medications that can hurt the liver, check the LiverTox database: https://www.ncbi.nlm.nih.gov/books/NBK547852.
-
2Drinking too much alcohol puts you at risk. Regular drinking can lead to a condition known as alcoholic fatty liver, which inflames your liver.[19] Unfortunately, this can lead to scarring, like fibrosis and cirrhosis.[20]
- If you stop drinking before any major scarring occurs, the alcoholic fatty liver can reverse on its own.
-
3Certain health conditions or family history may play a part. Check-in with your close relatives and see if anyone has a history of liver disease. If a close family member has ever had hemochromatosis, alpha-1-antitrypsin deficiency, or Wilson disease, you might be more at risk for liver issues.[21]
- At your annual doctor’s appointment, ask your physician to do a liver enzyme test. This is a great way to help you keep tabs on your liver health.
Advertisement
Question 5
Question 5 of 8:How can a doctor identify liver fibrosis?
-
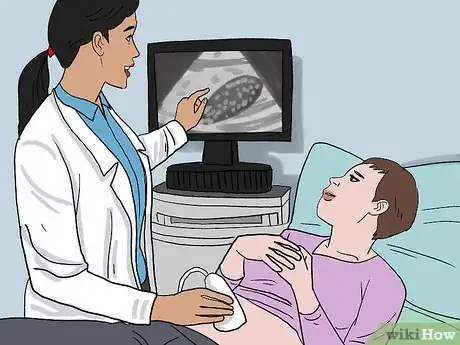
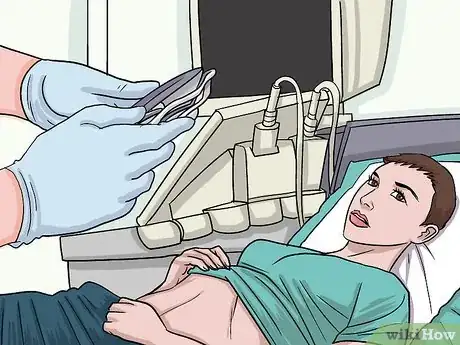
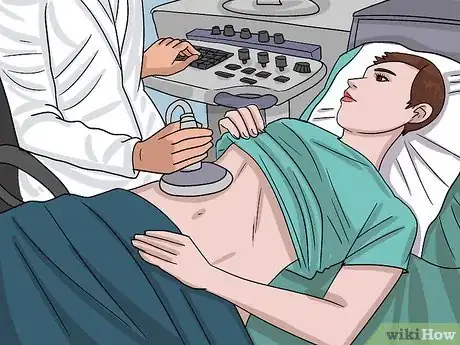
1A radiologist can perform an ultrasound or MRI elastography. In ultrasound elastography, radiologists study your liver with a probe and special sound waves, which help them determine where any scarring is. An MRI elastography locates scarring with an MRI machine and produces especially accurate results.[22]
-
2A doctor may take a biopsy. In a biopsy, a doctor collects samples of your liver with a thin needle. During the procedure, your doctor may collect up to 15 samples from different parts of the liver, so they perform more thorough testing. Unfortunately, this procedure can be pretty painful, and can only identify fibrosis in the small samples collected—not the entire liver.[23]
- A biopsy is a lot more invasive and painful than an elastography.
-
3Other imaging tests can help identify liver fibrosis. Abdominal ultrasounds and computed tomography (CT) scans are other non-invasive ways to identify scarred liver tissue. On an abdominal ultrasound and CT scan, scarred livers look a bit lumpier and smaller than a healthy liver.[24]Advertisement
Question 6
Question 6 of 8:Does liver fibrosis develop at a consistent rate?
-
1No, liver fibrosis can develop at different rates. Unfortunately, liver fibrosis doesn’t follow an exact timeline. Some people develop fibrosis slowly over several years, only to have scarring speed up later on. Other people can develop liver fibrosis very quickly—it really depends on the individual.[25]
Question 7
Question 7 of 8:What are the stages of liver fibrosis?
-
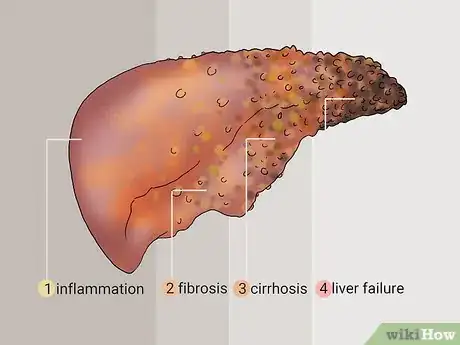
1Fibrosis is the second stage of liver damage. Liver damage is charted in 4 stages: inflammation (stage 1), fibrosis (stage 2), cirrhosis (stage 3), and liver failure (stage 4). During stage 2, your liver develops extra scar tissue but still works fairly normally. In cirrhosis, your liver is scarred all over and may not work properly.[26]Advertisement
Question 8
Question 8 of 8:Is liver fibrosis reversible?
-
1Research suggests that mild or moderate liver fibrosis is reversible. Some studies show that, with proper treatment for hepatitis C, patients can heal and recover completely from the fibrosis.[27] If you have liver fibrosis, talk with a doctor to figure out a specific treatment plan.
Expert Q&A
-
QuestionHow does liver fibrosis occur?
 Muhammad Khan, MD, MPHDr. Muhammad Khan is a Gastroenterologist, with over 10 years of experience. Dr. Khan specializes in Pediatric Gastroenterology, Hepatology, and Nutrition, and has a special focus in Therapeutic Endoscopy. He received his Bachelor’s, Master’s, and Doctorate of Medicine degrees from The University of Utah. Dr. Khan completed his residency training at Eastern Virginia Medical School, where he was inducted into the prestigious Alpha Omega Alpha honor society. He then completed his fellowship training at Lucile Packard Children’s Hospital at Stanford University. He is a Fellow of both the American Society of Gastrointestinal Endoscopy (ASGE) and the North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition (NASPGHAN).
Muhammad Khan, MD, MPHDr. Muhammad Khan is a Gastroenterologist, with over 10 years of experience. Dr. Khan specializes in Pediatric Gastroenterology, Hepatology, and Nutrition, and has a special focus in Therapeutic Endoscopy. He received his Bachelor’s, Master’s, and Doctorate of Medicine degrees from The University of Utah. Dr. Khan completed his residency training at Eastern Virginia Medical School, where he was inducted into the prestigious Alpha Omega Alpha honor society. He then completed his fellowship training at Lucile Packard Children’s Hospital at Stanford University. He is a Fellow of both the American Society of Gastrointestinal Endoscopy (ASGE) and the North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition (NASPGHAN).
Board Certified Gastroenterologist Ultimately, liver damage causes liver fibrosis—this damage can be severe and all at once, or over frequent, small amounts of time.
Ultimately, liver damage causes liver fibrosis—this damage can be severe and all at once, or over frequent, small amounts of time. -
QuestionWhat is the best way to avoid developing cirrhosis?
 Muhammad Khan, MD, MPHDr. Muhammad Khan is a Gastroenterologist, with over 10 years of experience. Dr. Khan specializes in Pediatric Gastroenterology, Hepatology, and Nutrition, and has a special focus in Therapeutic Endoscopy. He received his Bachelor’s, Master’s, and Doctorate of Medicine degrees from The University of Utah. Dr. Khan completed his residency training at Eastern Virginia Medical School, where he was inducted into the prestigious Alpha Omega Alpha honor society. He then completed his fellowship training at Lucile Packard Children’s Hospital at Stanford University. He is a Fellow of both the American Society of Gastrointestinal Endoscopy (ASGE) and the North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition (NASPGHAN).
Muhammad Khan, MD, MPHDr. Muhammad Khan is a Gastroenterologist, with over 10 years of experience. Dr. Khan specializes in Pediatric Gastroenterology, Hepatology, and Nutrition, and has a special focus in Therapeutic Endoscopy. He received his Bachelor’s, Master’s, and Doctorate of Medicine degrees from The University of Utah. Dr. Khan completed his residency training at Eastern Virginia Medical School, where he was inducted into the prestigious Alpha Omega Alpha honor society. He then completed his fellowship training at Lucile Packard Children’s Hospital at Stanford University. He is a Fellow of both the American Society of Gastrointestinal Endoscopy (ASGE) and the North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition (NASPGHAN).
Board Certified Gastroenterologist Focus on changing your diet and increasing your exercise regimen. In more extreme cases, geriatric surgery might be an option as well.
Focus on changing your diet and increasing your exercise regimen. In more extreme cases, geriatric surgery might be an option as well.
References
- ↑ https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3995196/
- ↑ Muhammad Khan, MD, MPH. Board Certified Gastroenterologist. Expert Interview. 24 August 2021.
- ↑ https://www.merckmanuals.com/home/liver-and-gallbladder-disorders/fibrosis-and-cirrhosis-of-the-liver/fibrosis-of-the-liver
- ↑ https://blog.radiology.virginia.edu/diagnosing-liver-fibrosis/
- ↑ Muhammad Khan, MD, MPH. Board Certified Gastroenterologist. Expert Interview. 24 August 2021.
- ↑ https://www.uhn.ca/PatientsFamilies/Health_Information/Health_Topics/Documents/Alcohol_and_the_Liver.pdf
- ↑ https://www.merckmanuals.com/home/special-subjects/recreational-drugs-and-intoxicants/alcohol
- ↑ https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6829586/
- ↑ https://www.cdc.gov/hepatitis/hcv/index.htm
- ↑ https://www.cdc.gov/hepatitis/hcv/cfaq.htm
- ↑ https://www.merckmanuals.com/home/liver-and-gallbladder-disorders/fibrosis-and-cirrhosis-of-the-liver/fibrosis-of-the-liver
- ↑ https://www.merckmanuals.com/home/liver-and-gallbladder-disorders/fibrosis-and-cirrhosis-of-the-liver/fibrosis-of-the-liver
- ↑ https://www.merckmanuals.com/home/liver-and-gallbladder-disorders/manifestations-of-liver-disease/fatty-liver
- ↑ https://www.mayoclinic.org/diseases-conditions/nonalcoholic-fatty-liver-disease/diagnosis-treatment/drc-20354573
- ↑ https://www.merckmanuals.com/home/liver-and-gallbladder-disorders/fibrosis-and-cirrhosis-of-the-liver/fibrosis-of-the-liver
- ↑ https://www.mayoclinic.org/diseases-conditions/hepatitis-c/symptoms-causes/syc-20354278
- ↑ https://www.hopkinsmedicine.org/health/wellness-and-prevention/5-reasons-you-may-be-at-risk-for-liver-disease
- ↑ https://www.ncbi.nlm.nih.gov/books/NBK547852/
- ↑ Muhammad Khan, MD, MPH. Board Certified Gastroenterologist. Expert Interview. 24 August 2021.
- ↑ https://www.hopkinsmedicine.org/health/wellness-and-prevention/5-reasons-you-may-be-at-risk-for-liver-disease
- ↑ https://www.hopkinsmedicine.org/health/wellness-and-prevention/5-reasons-you-may-be-at-risk-for-liver-disease
- ↑ https://blog.radiology.virginia.edu/diagnosing-liver-fibrosis/
- ↑ https://blog.radiology.virginia.edu/diagnosing-liver-fibrosis/
- ↑ https://www.radiologyinfo.org/en/info.cfm?pg=fatty-liver-disease
- ↑ https://www.hepatitis.va.gov/hcv/liver-fibrosis.asp
- ↑ https://blog.radiology.virginia.edu/diagnosing-liver-fibrosis/
- ↑ https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3995196/


















Medical Disclaimer
The content of this article is not intended to be a substitute for professional medical advice, examination, diagnosis, or treatment. You should always contact your doctor or other qualified healthcare professional before starting, changing, or stopping any kind of health treatment.
Read More...